Below is a description of the most common tests and procedures that are done either in our office or in the hospital
Allergy Skin Test
An allergy skin test is used to identify the substances that are causing the patient’s allergy symptoms. It is often performed by applying an extract of an allergen to your skin and then evaluating the skin’s reaction. The entire time for the skin test is about an hour at the maximum. The test does not hurt but if the patient has positive reaction to any allergen it is going to cause itching at the site of the test. Systemic reactions to skin testing with low blood pressure, difficulty breathing or rash are extremely rare.
Please refer to the patients forms for the medications that should be avoided before the skin test is done. Make sure to review all the medicines that you are taking including any over the counter medicines with our medical staff before performing the test.
- Scratch test (prick test). We perform the skin test in our practice on an area of the patient’s back. Areas on your skin are then marked with a pen to identify each allergen or each allergens panel (A, B, etc.) that will be tested. A disposable pricking device is then used so the extract can enter into the outer layer of the skin, called the epidermis.
- Intradermal test. A small amount of the allergen is injected just under the skin.
When the allergy skin test is over the skin is clean with alcohol. A mild cortisone cream may be applied to the test site to relieve any excessive itching.
Call 911 immediately if you experience any of the following symptoms: dizziness or lightheadedness, wheezing, shortness of breath, rash, swelling of the face, lips or mouth, or difficulty swallowing.
Bronchoscopy With EBUS
Bronchoscopy is a procedure that allows your doctor to look at your airway through a thin viewing instrument called a bronchoscope. During a bronchoscopy, your doctor will examine your throat, larynx, trachea, and lower airways.
There are two types of bronchoscopes:
A flexible bronchoscope: It is a long, thin, lighted tube and it is the most commonly used type.
A rigid bronchoscope is usually done with general anesthesia and it is a straight, hollow metal tube.
Bronchoscopy may be used for many different reasons like if you have hemoptysis (coughing up blood) to locate the source and control the bleeding if possible; to do washing of the airways; to remove any aspirated foreign body; to take tissue samples from a tumor, lymph nodes or any abnormal lungs or to resect a tumor in the airway.
The most common complications of the procedure include bleeding, pneumothorax (air leak and collapsed lung) and infection. They are rare. Death from bronchoscopy is very rare.
To prepare for bronchoscopy:
- 1. You should not eat or drink for at least 8 to 10 hours before the procedure.
- 2. You need to arrange to have someone drive you home after the procedure.
- 3. You should stop Plavix, Brilinta & Effient 7 days before the procedure.
- 4. You should stop Coumadin, Xarelto, Eliquis & Pradaxa at least 3 days before the procedure.
Before the procedure, your eyes will be covered to protect them and a mouth piece (bite block) will be in your mouth to protect the bronchoscope.
During this procedure, you will lie on your back on a table however sometimes the procedure is done while you are sitting upright. You will be given medications to help you relax and make you sleepy during the procedure.
C-Shaped X-ray machine may be placed above you to transmit an X-ray picture to a TV monitor.
The bronchoscopy usually takes between 30 to 60 minutes. You will be in recovery for 2 to 3 hours after the procedure.
When you go home you should call your doctor if you have fever, chest pain, or coughing up blood.
Endobronchial Ultrasound (EBUS)
Endobronchial ultrasound (EBUS) is a minimally invasive method of diagnosing lung cancer, infections, and other inflammatory diseases. EBUS enables doctors to obtain tissue or fluid samples from the lungs and surrounding lymph nodes.
Why is EBUS used?
EBUS allows physicians to perform a technique known as transbronchial needle aspiration (TBNA) to obtain tissue samples from the lungs and surrounding lymph nodes without conventional surgery. The samples can be used for diagnosing and staging of lung cancer, detecting infections, and identifying inflammatory diseases that affect the lungs, such as sarcoidosis or cancers like lymphoma.
What makes EBUS different?
- The physician can perform transbronchial needle aspiration (TBNA) using a bronchoscope inserted through the mouth
- No incisions are necessary
- It provides real-time imaging.
- No incisions are necessary
- A rapid onsite pathologic evaluation (ROSE) in the operating room can process and examine biopsy samples as they are obtained.
- EBUS is performed under moderate sedation or general anesthesia
- Patients recover quickly and can usually go home the same day
Home Sleep Test (HST)
Oximetry
Pulmonary Function Test (PFT) (Spirometry, Lung volume, DLCO)
Spirometry
Spirometry measures the amount of air a person can breathe in and out as well as the speed of air movement to and from the lungs. Several different maneuvers are usually performed:
The Forced Vital Capacity (FVC) requires you to take a deep breath and blow into a tube as hard and long as you can (like blowing a trumpet.) This is a sensitive test for obstructive lung disease like asthma or emphysema. The Maximal Voluntary Ventilation (MVV) requires you to huff and puff through a mouthpiece, breathing as much as you can for about 10 seconds. This procedure measures lung flexibility and muscle strength.
These procedures are usually repeated several times after a short rest, to assure consistency and accuracy. These tests take only a few minutes each, and may be repeated after the use of an inhaled medication (bronchodilator) to test for the presence of asthma.
Lung Volumes
The amount of air that your lungs can hold cannot be measured simply by blowing out. Instead, it must be measured indirectly by one of two methods:
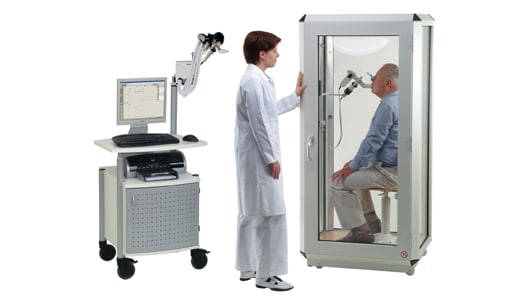
Body Box (Plethysmograph)which is recommended by the American Thoracic Society and that is what we use in our practice In this procedure, you sit in a Plexiglas box about the size of a telephone booth and breathe in and out through a small mouthpiece. On the technologist’s prompt, you pant like a puppy for 2 or 3 seconds while the box is closed. With the help of data from the spirometry test (below), the instrument instantly calculates your lung volume.
The Nitrogen Washout Test uses simpler equipment, but gives the same results. By breathing pure oxygen through a mouthpiece, all the nitrogen in your lungs (normal air is 78% nitrogen) is replaced with oxygen. The system measures the amount of gas removed and calculates lung size from this data. The test takes no more than seven minutes.
Diffusing Capacity (DLCO)
The DLCO tests the ability of air to cross through your lungs and into your blood stream without actually drawing any blood. After taking a deep breath of normal air mixed with a tiny bit of harmless but rare gas, you are asked to hold your breath for ten seconds. After you exhale, this test determines how much of the rare gas passed into your blood, indicating how well oxygen gets in and carbon dioxide gets out. The DLCO test is very helpful in differentiating emphysema from other obstructive diseases.
Six Minute Walk Test
This test measures the distance that a patient can quickly walk on a flat, hard surface in a period of 6 minutes (the 6MWD).
1. INDICATIONS:
- 1. The strongest indication for the 6MWT is for measuring the response to medical interventions in patients with moderate to severe heart or lung disease.
- 2. The 6MWT has also been used as a one-time measure of functional status of patients.
- 3. The 6MWT has also been used as a predictor of morbidity and mortality.
2. CONTRAINDICATIONS:
Absolute Contraindications:
- 1. Unstable angina during the previous month.
- 2. Myocardial infarction during the previous month.
Relative Contraindications (Call ordering doctor before you proceed):
- 1. Resting heart rate of more than 120.
- 2. Systolic blood pressure of more than 180 mm Hg.
- 3. Diastolic blood pressure of more than 100 mm Hg.
Sleep Study (Polysomnography, PSG)
1. Polysomnography PSG:
What is a Sleep Study?
A Sleep Study or Polysomnogram (PSG) is a multiple-component test, which electronically transmits and records specific physical activities while you sleep. The recordings become data, which will be “read” or interpreted by a qualified physician to determine whether or not you have a sleep disorder.
What to Bring With You?
Pack a small bag with your pajamas (preferably two pieces), a toothbrush and any other items you will need the next morning. Many patients like to bring their own pillow for better sleep. In the sleep lab, you have a private bedroom that resembles a hotel room or your bedroom at home. For safety purposes, we do not provide showers. Once you arrive, you will be asked to slip into your pajamas before the process of hooking up the surface electrodes (leads) begins. The hook-up process may take place in your bedroom or an outer work area. Setup can take 30-45 minutes in order to get everything connected properly. The electrodes are temporarily “glued” to your skin and scalp but don’t worry, the glue comes off easily the next morning! Once the electrodes and all other components are in place, you are asked to go to bed to sleep. The data that is collected and recorded from these electrodes is what makes a polysomnographic study. Although being hooked up may look uncomfortable and sleeping through the night seems impossible, most patients fall asleep with little difficulty. Televisions may be provided, but you may want to bring a book or magazine.
A key part of a sleep study is understanding what is happening while you sleep. By attaching the electrodes to your body, the recorded electrical signals generated by your brain, heart, airflow, eye movement, and muscle activity are sent back through the wires and recorded digitally. The pattern of this activity can be recognized by a sleep specialist who “reads” or interprets the study. These valuable clues reveal whether or not you have a sleep disorder, and if present, how severe it is.
The EEG, or electroencephalogram, is a major part of a sleep study. It measures and records four forms of brain wave activity – alpha, beta, delta and theta waves. Each stage is recognized by the presence and percentage of these waves. Sleep is divided into REM (Rapid Eye Movement) and NREM (Non Rapid Eye Movements) sleep (stages 1-4).
The EMG, or electromyogram, records muscle activity such as face twitches, teeth grinding, and leg movements. It also helps in determining the presence of REM stage sleep. The amount and duration of these activities provides the doctor important information about your sleep.
The EOG, or electro-oculogram, records eye movements. These movements are important in determining the different sleep stages, particularly REM stage sleep. The electrodes are usually placed on the outer aspect of your right eyebrow and along the outer aspect below or beneath your left eye.
The EKG, or electrocardiogram, records heart activities, such as rate and rhythm. Electrodes are placed on your chest.
The Nasal Airflow Sensor records airflow to help recognize apnea and hypopnea events. A sensor is placed near your nose and mouth.
The Chest/Abdomen Belts record breathing depth and to help recognize apnea and hypopnea events. Elastic belts are placed around your chest and abdomen.
The Oximeter records blood oxygen saturation. A band-aid like clip is placed on a finger.
The Snore Microphone records snoring. An electrode is placed over your trachea, on your lower neck.
Sleeping is a complex activity that must occur for a successful polysomnographic study. During sleep, our brain and body cycle between NREM and REM sleep approximately every 90 minutes.
During these transitions, major changes occur in our EEG, EOG, EMG, heart rate and respiration that are necessary for healthy sleep. If abnormal changes are observed during a particular sleep stage, then we are able to define this problem as it occurs during the night.
Some sleep disorders are generally worse in a particular sleep stage, such as sleep apnea during REM sleep and PLMD in NREM sleep. Your PSG technician and sleep specialist are well aware of these facts and want you to get as good a night’s sleep as possible in order to make your test experience as fruitful as possible.
Once the sleep specialist reads the “book” of data, they will know if you have a sleep problem or a sleep disorder. Following a diagnosis, the sleep specialist will work with you and your doctor to plan appropriate treatment.
CPAP/BiPAP therapy is the first line of treatment for sleep apnea. The CPAP device delivers pressurized air through tubing to a mask (nasal, full-face, or nasal pillows) which are fitted around the head. The pressurized air acts as an airway splint. It gently opens the patient’s throat and breathing passages, allowing them to breathe normally while asleep.
To properly treat sleep apnea, the correct CPAP device air pressure setting must be determined by titration. Titration is done for each patient – there is no “one size fits all” solution.
2. Polysomnography with CPAP Titration:
A CPAP/BiPAP Titration is required if sleep apnea is diagnosed. During a titration study, the patient will sleep just like a normal sleep study, but they will also wear a nasal mask which is connected to a CPAP machine. The technician will set the air pressure on the CPAP device at a certain level and gradually increase the pressure to eliminate the obstructive sleep apnea. This process continues throughout the night until the optimum pressure is reached.
After the titration study, the ‘book’ of data is again read and interpreted by the sleep specialist. Based on the study, the sleep specialist will determine the appropriate pressure for the CPAP machine. The sleep lab will then order your CPAP machine for you!
3. Multiple Sleep Latency Test (MSLT):
For patients that have excessive sleepiness, a MSLT or (Multiple Sleep Latency Test) may be ordered. This is a daytime nap study that measures how quickly you fall asleep and how quickly you go into REM sleep or dream sleep. This study requires you take a series of naps throughout the day following a PSG study. You will be asked to abstain from caffeinated products during this study and remain awake between naps. Since you will be at the lab all day, please bring a book to read, your laptop, or something to help you stay awake between the naps. Also bring your normal medications unless your physician tells you otherwise.
